GLAUCOMA AND ITS MANAGEMENT

What is Glaucoma?
Glaucoma is a serious eye condition which is characterized by progressive and irreversible damage to the optic nerve and which if untreated can lead to blindness.

Though the raised pressure of the eye is a crucial factor for identifying glaucoma, people can develop glaucoma even with the normal pressure of the eye.
Worldwide, glaucoma is the second leading cause of blindness. In India, glaucoma is the leading cause of irreversible blindness.
Managing Glaucoma
It is appalling to know that more than 90 percent of cases of glaucoma remain undiagnosed in the community. The management and treatment depend upon how early the disease is diagnosed and the treatment is started. With the irreversible damage that the disease does, the management could slow down the progress and help the patient in preventing total blindness. Here are few tips for robust management.
- Treatment Adherence
The glaucoma treatment is done to prevent any further vision loss. Any treatment cannot restore vision that is already lost through glaucoma, but the further loss of sight can be either prevented or slowed.

At present, the only recognized treatment for glaucoma is to lower the eye pressure majorly with the use of eye drops. Irregularity in administrating eye drops or medication could increase the eye pressure and risk of progressive loss of sight. It is important here to note that it’s important to follow the routine that has been planned for you as management for each case is different. In case when the drops do not reduce the eye pressure as needed, there are other options such as laser therapy or surgery.
- Regular Monitoring

The Intraocular pressure inside the eye could keep changing because of many conditions including the ongoing treatment. A regular assessment of the changes to the optic nerve and peripheral vision is needed. The treatment and management plan may have to be reviewed to ensure further damage to the optic nerve does not occur.
The intervals needed between the follow-up appointments are different for each case. The ophthalmologist determines the frequency of the follow-up appointments based on the individual case and the outcome of the initial appointment.
Any activity undertaken or avoided for glaucoma management must be done under an ophthalmologist’s guidance.
Glaucoma Surgery
If any treatment for glaucoma fails to cure or manage glaucoma then the surgery could be suggested. Surgery for glaucoma can help lower the pressure in the eye. It is important to note that the surgery cannot cure glaucoma or even undo vision loss, but it can certainly help protect the vision and stop it from getting worse.
The different types of Glaucoma surgeries are:
- Trabeculectomy
Trabeculectomy surgery is done to treat open-angle glaucoma. The extra fluid in the eye, which is causing the pressure, is drained by creating a tiny cut in the eye. The surgery is short and the patient can go home the same day.
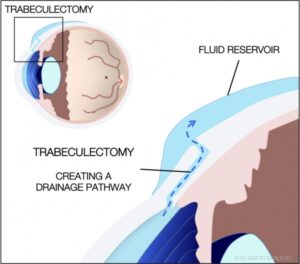
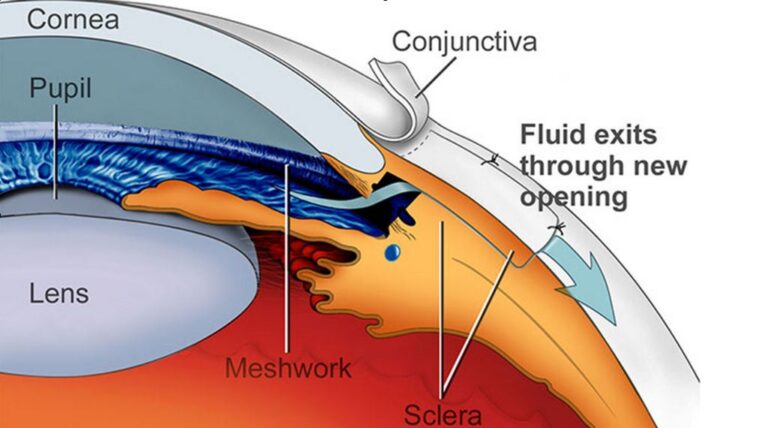
- Glaucoma Implant Surgery
Glaucoma implant surgery is used to treat several types of glaucoma such as congenital glaucoma, neovascular glaucoma, and glaucoma caused by an injury. It involves implanting a tiny tube to drain extra fluid lowering the eye pressure.

- Minimally Invasive Glaucoma Surgery or MIGS

The minimally invasive approach is an advanced method using techniques that cause minimal cuts and scaring and hence faster recovery.
Post-surgery, eye drops or eye ointments could be recommended to prevent swelling and infections. Restrictions on some activities for few weeks along with regular check-ups are advised.
YAG Laser Peripheral Iridotomy
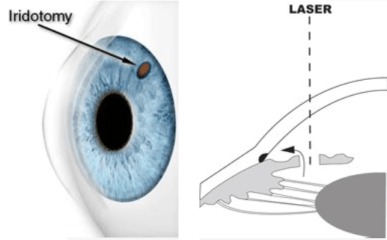
Laser peripheral iridotomy is a medical procedure that is commonly used to treat primary angle‐closure glaucoma, patients who are primary angle‐closure suspects and even eyes with secondary causes of iridocorneal angle-closure.
The procedure uses a laser device to create a hole in the iris which allows aqueous humor to traverse directly from the posterior to the anterior chamber and thus relieving a pupillary block. The tiny opening allows an opening up of the angle of the eye. The narrow or closed-angle thus becomes an open-angle.
The procedure is performed using topical anesthesia. Generally, there is no pain experienced after the procedure is done. The procedure is very short and is completed with the patient seated at the laser with no sedation required.
